Koumenis Andreas,1 Dimitrakopoulou Evangelia,1 Karafotaki Kyriaki,1 Draghi Athanasia,1 Vardiampasi Anna,2 Filippou Dimitrios,3 Troupis Theodore,3 Kaklamanos Ioannis,1 Mariolis – Sapsakos Theodoros1,4
1 University Surgical Clinic, General and Oncological Hospital of Kifisia “Oi Agioi Anargiroi”, Athens, Greece
2 2nd Pathology Clinic, General and Oncological Hospital of Kifisia “Oi Agioi Anargiroi”, Athens, Greece
3 Department of Anatomy, School of Medicine, NKUA, Athens, Greece
4 Anatomy, Embryology and Histology Lab, Faculty of Nursing, NKUA, Athens,Greece
Correspondence Address: Andreas Koumenis, a_koumeni@icloud.com
Abstract
Nasogastric tube (NGT) insertion for either enteral feeding or gastric decompression is a common and generally considered safe procedure. [1-I]. There have been some reports of alimentary tract perforation mainly in neonates and infants, with only sparse reports of perforation in adults. Here, we present a case of early postoperative leakage attributed to perforation from the NGT inside the gastric remnant.
Introduction
Subtotal gastrectomy is the procedure of choice for tumors located in the lower part of the stomach. A rare and not-so-often thought-of complication may arise from the postoperative use of a nasogastric drainage tube. In this case report, we present a case of a gastric remnant perforation due to pressure from a nasogastric tube looping inside the gastric remnant following subtotal gastrectomy and D2 lymph node resection in a 74-year-old. We aim to emphasize the potential complications associated with the use of NGT postoperatively and the importance of careful patient monitoring to proceed to prompt intervention if the need arises. To our knowledge, this is the first reported incident of a gastric remnant perforation from an NGT loop pressuring the gastric wall.
Case Presentation
A 74-year-old female presented at our clinic for a scheduled subtotal gastrectomy and D2 lymph node resection after being diagnosed with Lauren diffuse type gastric adenocarcinoma located at the distal- third of the lesser curve of the stomach. She had no significant medical history apart from hypertension and dyslipidemia and she had no previous surgeries to declare. Her body mass index (BMI) was 38 kg/m2.
She received preoperative mechanical bowel preparation as well as prophylactic antibiotic coverage with cefuroxime/metronidazole as per our clinic’s protocol.

Figure1: surgical side after subtotal gastrectomy and D2 lymph node resection with the gastric remnant visible
The surgeon chose an open approach, and an upper midline incision was performed extending from the xiphoid to approximately 3cm below the umbilicus. The palpable mass was confirmed to be at the lower 1/3 of the stomach, so a subtotal gastrectomy was the procedure of choice. After meticulous dissection, the stomach was divided from high on the lesser curve of the stomach up to the middle of the greater curve, and a Roux-en-Y reconstruction of the gastrointestinal tract was performed. The gastrojejunal anastomosis was performed with a circular stapler reinforced by interrupted full thickness polyglactin sutures. The duodenal stamp’s staple line was also reinforced with interrupted sutures as was the gastric staple line. Two closed drains were placed, one at the side of the duodenal stamp and the other at the side of the gastrointestinal anastomosis.
Intraoperatively, a 16Fr Polyvinyl Chloride (PVC) NGT was placed by the anesthesiologist and the surgeon assisted transabdominally for postoperative decompression and prevention of aspiration taking into consideration that a post-operative blind placement if an NGT was needed would be difficult and associated with added risk due to the nature of the surgery.
During the procedure, the short splenic arteries above the proximal half of the greater curve remained untouched and the remnant stomach above the line of dissection remained with no manipulations and no stay sutures were used due to the relatively large size of the remnant.
Eighteen hours after surgery the patient complained of epigastric pain which radiated the right upper quadrant. On clinical examination she was afebrile, and her heart rate was 80 bpm and blood pressure 140/80 mm Hg. Right upper quadrant and epigastric tenderness were present on palpation, without rebound or percussion tenderness. Her laboratory tests showed: C reactive protein 11.34 mg/dL, a white cell count of 13.32 K/L, and a hemoglobin level of 11.7 g/dL.
Two hours after the initial assessment, greenish turbid fluid presented in the drainage tube – no more than 5-6ml. Re-evaluation of the patient presented mild rebound tenderness and localized peritonitis. An abdominal computer tomography (CT) scan with water-soluble oral contrast was ordered which revealed a contrast leak near the left subphrenic space. The nasogastric tube was visible forming a loop inside the gastric stump and in closed contact with the gastric wall. An emergency laparotomy was deemed necessary to investigate the cause of the leak and prevent the development of diffuse peritonitis.
Figure2,3: CT scan showing the NGT looping inside the gastric remnant |
The initial incision was reopened and after the first assessment, both the duodenal stump incisional line and the two anastomotic sides of the Roux – en -Y anastomosis were intact. The leak was due to a perforation of the gastric remnant at the gastric fundus near the cardiac notch. Inside the gastric remnant, the nasogastric tube was visible through the deficit forming a loop with the convex section exerting constant pressure on the gastric wall. Taking into consideration that no surgical dissections or handlings were performed at that region and the visible pressure on the gastric wall from the NGT loop, the gastric perforation could only be attributed to the NGT.
After debriding of the perforation side, a primary repair was performed, and the defect was primarily closed with Vicryl 2-0 suture. Extensive abdominal washout followed and the drainage tubes were replaced. The abdominal wall was closed with a PDS no1 loop suture.
The patient had an uneventful recovery with the time of the first flatus being the second postoperative day and the patient starting oral feeding on the third postoperative day. The discharge was nine days after the first surgery, and she has a steady recovery at 12-month follow-up period.
Discussion
Gastric perforation is a life-threatening cause of acute abdomen which can either be traumatic, ischemic or spontaneous, with the most common cause being spontaneous perforation due to peptic ulcer disease. Ιatrogenic causes of spontaneous gastric perforation such as nasogastric tube (NGT) and orogastric tube placement are extremely rare although these intubations are frequently performed in surgical patients.
In the adult population, oesophageal and pharyngo-oesophageal perforation is more common as a nasogastric tube placement complication than gastric perforation, which is more common in pediatric population
Ghahremani et al described a series of six cases with gastric perforation after NGT placement and documented salicylate use, gastric anastomosis, and metastatic gastro-oesophageal cancer as potential risk factors. [2-A].
There are also reports in the literature of gastric perforation from NGT placement in elderly patients or patients with connective tissue disorders [2-A,3-B,4-C,5-G] and to patients who had undergone surgery [6-D,7-E]. Daliya et al presented a case of gastric perforation in a 32-year-old male from NGT intubation after laparotomy for acute intraabdominal bleeding, [3-B] and Lee et al a 63-yar-old patient with gastric perforation after NGT placing for feeding. [4-c] Van Dinter et al report a case of gastric perforation in a female patient nine years after Roux-en-Y gastric bypass. [6-D] and Morell et al, a 39-year-old patient with a history of gastric sleeve surgery and rupture after intra-operative NGT placement for thyroidectomy [7-E].
|
To our knowledge, this is the first reported case of a gastric remnant perforation from an intraoperative placed NGT after subtotal gastrectomy.
The exact mechanism of perforation is not clarified, but taking into consideration that surgical manipulation was performed near the perforation site, the local blood supply was not compromised and a clear coiling of the NGT was visible through the perforation deficit with the tube actively pressuring the gastric wall, the evidence suggests that the perforation was directly linked to the NGT. We theorize that the NGT may have been dislocated during extubation, causing the formation of a rigid loop inside the gastric remnant. In literature, size, stiffness and tendency of NGT material such as polyethylene, polyvinyl chloride or latex to interact with gastric acid and become more rigid have been flagged as possible contributing factors of gastric wall erosion [4-c]
Most often, postoperative leakage after gastric surgery is due to anastomotic side leak from any side with a staple line or sutures and occurs between 5 and 10 days after surgery. The incidence of leakage in literaturee ranges between 0 and 17%, and mortality increase due to the leakage is reported. The patient will present mostly with tachycardia, hypotension, and abdominal pain up to acute abdomen. The treatment depends on the severity of the clinical presentation.
Figure5: The intact gastrojejunal anastomosis |
Conservative treatment can be considered in stable patients with broad-spectrum antibiotics, nutritional support, and fluid infusion whereas an unstable patient requires an exploratory laparotomy and closure of the leakage site. In our case, the early leakage (<72 h after the operation) and the onset of signs of peritonitis deemed the surgical re-intervention necessary with the aim of potential direct closure of the leakage. [8-H]
The prophylactic use of NGT for decompression, reduction of aspirational risk from nausea and vomiting, and prevention of postoperative distention due to paralytic ileus, thus improving anastomotic safety, have been shown as nonbeneficial in various metanalysis [9-J]. Despite that, many surgeons continue to use NGTs in the early postoperative period after gastric resection, in cases where anew placement may be difficult or associated with added risks, such as prior gastric or bariatric surgery, hiatal hernia, esophagotomy, or in patients who may not be able to cooperate postoperatively[10-F]. In our case, the added risk of an injury from a blind placement and the extensive dissection needed for the D2 lymphadenectomy that undeniably affects intestinal motility after surgery contributed to the decision to keep the NGT postoperatively.
Conclusion
The case presented is a rare cause of early leakage after subtotal gastrectomy that was attributed to NGT perforation of the gastric remnant. This case report highlights the potential complications associated with the use of NGT postoperatively and the importance of careful patient monitoring to proceed to prompt intervention if the need arises. Although extremely rare, the surgeon must be aware of the risk of NGT perforation both during the placement but also after the extubation of the patient. Close monitoring and early intervention in case of diffuse peritonitis is also vital.
References
- Metheny, N. A., Meert, K. L., & Clouse, R. E. (2007). Complications related to feeding tube placement. Current opinion in gastroenterology, 23(2), 178–182. https://doi.org/10.1097/MOG.0b013e3280287a0f
- Ghahremani, G. G., Turner, M. A., & Port, R. B. (1980). Iatrogenic intubation injuries of the upper gastrointestinal tract in adults. Gastrointestinal radiology, 5(1), 1–10. https://doi.org/10.1007/BF01888590
- Daliya, P., White, T. J., & Makhdoomi, K. R. (2012). Gastric perforation in an adult male following nasogastric intubation. Annals of the Royal College of Surgeons of England, 94(7), e210–e212. https://doi.org/10.1308/003588412X13171221502347
- Lee, S. H., Kim, M. S., Kim, K. H., Do, J. Y., Park, J. W., Kim, T. N., & Yoon, K. W. (2007). Gastric Perforation Caused by Nasogastric Intubation in a Patient on Peritoneal Dialysis. Korean Journal of Nephrology;: 250-253, 2007. https://pesquisa.bvsalud.org/portal/resource/pt/wpr-27809
- Janicki, A., Van Ginkel, C., & Cohn, J. (2015). Gastric Perforation Following Nasogastric Intubation in an Elderly Male. Rhode Island medical journal (2013), 98(9), 45–46.
- Van Dinter, T. G., Jr, John, L., Guileyardo, J. M., & John S, F. (2013). Intestinal perforation caused by insertion of a nasogastric tube late after gastric bypass. Proceedings (Baylor University. Medical Center), 26(1), 11–15. https://doi.org/10.1080/08998280.2013.11928900
- Morrell D., Witte R. S., Bello G., Rogers M. A., Pauli M. E. (2020) Nasogastric tube perforation masquerading as a delayed gastric sleeve leak : Bariatric Times. https://bariatrictimes.com/ngt-perforation-delayed-gastric-sleeve-leak/
- Hummel, R., & Bausch, D. (2017). Anastomotic Leakage after Upper Gastrointestinal Surgery: Surgical Treatment. Visceral medicine, 33(3), 207–211. https://doi.org/10.1159/000470884
- Yang, Z., Zheng, Q., & Wang, Z. (2008). Meta-analysis of the need for nasogastric or nasojejunal decompression after gastrectomy for gastric cancer. The British journal of surgery, 95(7), 809–816. https://doi.org/10.1002/bjs.6198
- Hodin RA. Inpatient placement and management of nasogastric and nasoenteric tubes in adults. In: UpToDate, Connor RF (Ed), Wolters Kluwer. (Accessed on June 7, 2024.)

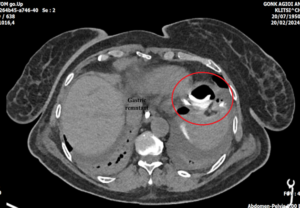

 Figure 4: the side of the gastric remnant perforation
Figure 4: the side of the gastric remnant perforation